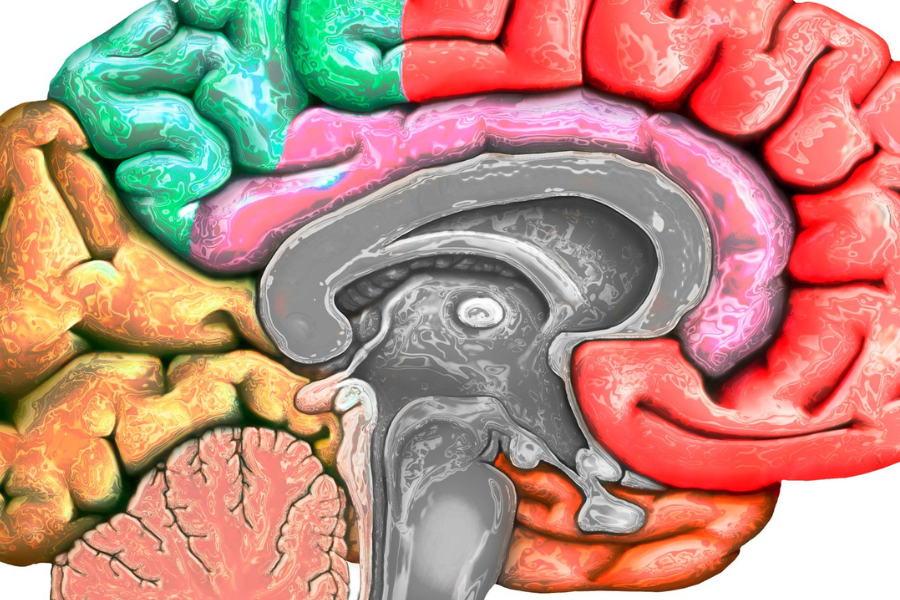
The thalamus is composed of two structures (left and right) in the brain that together play a significant role in our body. The thalamus is not only part of our body’s central nervous system which is composed of our brain and spinal cord, but it is also a part of our limbic system which has several functions such as our emotions, memory, behavior, and motivation. It is primarily known as the relay center of our body for all sensory (with the exception of smell) and motor information, and also plays a major role in our consciousness, alertness, sleep and wakefulness. It sends out information through relay stations, known as tracts, that transmit information to and from structures called nuclei. There are many nuclei for different types of functions such as feeling touch or pain. The thalamus is also the gatekeeper of these signals, in a sense that it is making sure the information is being sent to its proper destination.
The thalamus can receive information from many parts of the body where it receives, analyzes, relays the information to the appropriate destination in the cerebral cortex. For example, the thalamus receives visual sensory information from the retina of our eyes, processes the information, and would send it to the brain lobe responsible for vision (occipital lobe), where it is further processed. In other instances, it can send information it receives to a widespread area in our cortex for more general functions such as alertness. Additionally, the thalamus relay centers are bidirectional, meaning that information can be sent back to the thalamus to fine tune information.
Retrieved from:https://ranzcrpart1.fandom.com/wiki/Grey_matter_nuclei_(non-cranial_nerve):Thalamus?file=Parts-of-the-brain-thalamus.jpg
The thalamus can be broadly classified into six major functional components:
| Functional Class
*Note: within these classes lie multiple nuclei responsible for functions |
Function(s) |
| Reticular Nuclei |
- Arousal
- Synchrony and rhythms of thalamic neuronal activity
- A role in epileptogenesis (developing seizures)
|
| Intralaminar Nuclei |
- Arousal
- Attention
- Nociception (components of pain)
|
| Limbic Nuclei |
- Mood
- Emotional experience and expression
- Motivation
- Learning
- Memory
- Drive
|
| Specific Sensory Nuclei |
- Auditory
- Visual
- Gustatory
- Vestibular
- Somatosensory body and limbs
- Somatosensory head and neck
|
| Effector Nuclei |
- Movement (Motor)
- Complex behaviors
- Motor programming
- Aspects of language
|
| Associative Nuclei |
- High level cognition (executive functions)
- Working memory
- Higher order somatosensory and visual spatial integration
- Spatial cognition
- Likely involved in goal directed reaching and conceptual and analytical thinking
- Attending to visual stimuli
- Drive
- Motivation
- Inhibition
- Emotion
|
Damage to the thalamus depending on the location of the lesion could include the following symptoms:
| Impairment |
Strategies |
| Anterograde amnesia
|
- Using a desk calendar or phone calendar (make it a habit to check it every morning and glance at it throughout the day)
- Setting reminders on your phone
- Setting alarms on your phone
- Writing notes on post it notes and please them on visible areas such as your laptop
- Use a notepad to cross off your daily checklist
- Using a dry erase board in room or on your refrigerator for important information
- Placing important objects in your sight
- Eating a nutritious diet
- Abstain from drinking alcohol
|
| Aphasia
|
- Use pictures or drawing boards to communicate needs
- Minimize distractions and background noise
|
Agnosia
- Inability to recognize information such as objects or familiar faces
|
- Performing tasks in a predictable environment (e.g., placing clothing in the same location every morning)
- Follow a consistent routine as much as possible
- Adapt the environment with the most commonly used items in sight.
- Declutter irrelevant items
- Look for clues, or differences in faces, such as a birthmark
|
Ideomotor apraxia
- Difficulty carrying out purposeful movements
|
- Using visual pictures to sequence through steps such as putting on a shirt
- Using dycem to help items such as plates and cups not slip
- Performing activity in their usual environment
- Limit distractions
- Allow individuals to make mistakes to learn
|
| Tremors |
- Using weighted item to help reduce tremors
- Weighted cuffs on wrist
- Weighted vest
- Weighted utensils, drinkware, plates
- Using adaptive equipment to reduce spills while eating
- Plate guard
- Scoop dish
- Using a “steady spoon”
- Placing dycem to help keep items in place
- Making sure your core and lower body are stabilize (button on your seat, feet placed firmly on the floor) to have more control of your arms, neck and head
- Using your peripheral vision can help with tremors
- Increasing textures (e.g., dycem around utensil) to help grasp objects better
- Overshoot for items to pick them up (scoop) on the way back
- Use single joints instead of multiple joints (e.g., elbows placed firmly on table while using your wrist and hands)
|
| Visual field loss
|
- Ophthalmologist might recommend prismatic correction glasses to help with double vision
- Patching one eye
- Practice scanning techniques to check for blind spots
|
Spatial deficits
- Difficulty judging distances
|
- Overshoot for items to scoop them back to you if having difficulties judging the item’s distance
- Using bright tape on stairs to know where to step or doorways
- Helpful to place on the edges of bathtubs or sinks to stand out
- High contrast colors in your environment such as bathrooms to make items stand out
|
| Loss of Temperature Sensation |
- Use unaffected hand to check temperatures such as the shower before getting in
- Permanently setting your water heater to a safe temperature
- Looking for clues such as steam
|
| Loss of Sensation to Pain or Touch |
- Make it a habit to constantly perform skin checks on areas of body that does not feel pain
- Checking for any redness on bony prominences of the body (e.g., buttox, toes, ankles)
- To reduce possibility of pressure sores
- Every morning and night
- Every time after showering
- See Hemiplegia section for similar tips
|
Hemiplegia
- Paralysis on one side of the body
|
- Engage in self range of motion exercises to decrease possibility of contractures and to increase sensation to the affected side
- Place your body weight on affected side as much as possible to help regain function
- Lying your arm out on table during activities
- Shifting your weight on your affected side while sitting
- Feet place firmly on floor
- Using affected limb as much as possible to help with task to provide input
- Examples include placing jar against affected hand to help stabilize while your other hand helps open it
- Using one handed dressing methods
- Adaptive equipment such as reachers
|
Hemiparesis
- Weakness on one side of the body
|
- Complete tasks while seated to conserve energy
- Taking plenty or rest breaks
- Engage affected head as much as possible to gain strength (e.g., when showering using a hand over hand method to assist affected hand while washing hair)
- Safety: using assistive device for balance
|
| Aggression or Agitation |
- Minimize confusion
- Use short simple words
- Utilizing coping strategies (Deep breathing exercises meditation. Videos can be found on online such as Youtube)
- Journaling to discover patterns of triggers before experiencing anger
- Practicing counting down from 10 before reacting
- Walking away from the situation instead of engaging in behavior
- Listening to music to increase mood
- Aroma therapy such as lavender oil
- Keep the environment safe!
- Remove dangerous objects
|
| Apathy |
- Engaging in music or art therapy
- Studies have also shown pet therapy may have a positive effect on apathy
- Getting a good night’s rest
- Aroma therapy (e.g., lavender oils)
- Breaking activity in smaller tasks to increase success
- Engaging in exercise
- Joining a support group
|
| Fluctuating Arousal and Orientation |
- Getting a good night’s sleep
- Provide extra stimulation for alertness (e.g., scents) or reduce stimulation as needed
|
| Perseveration behaviors |
- Give constant feedback to bring awareness. For example, saying “You just asked that. We just let you know your sister is on her way”
- Redirect individual – “Let’s have you brush your teeth now”
|
| Sleep disorders |
- Make sure you do not have a heavy meal a few hours before bed
- Use blue light glasses while using phone or computer at night
- Aroma therapy (Lavender oils)
- Refraining from technology use once lying in bed
- Using a sleep diary (can be printed online) to track sleeping patterns
- Limit caffeine intake
- Decaf coffee (note: decaf still has caffeine)
- Teas with NO caffeine
- Chamomile tea with lavender
|
References:
Torrico T.J., & Munakomi, S. (2020). Neuroanatomy, thalamus. StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK542184/
Schmahmann, J.D., Pandya, D.N. (2008) Disconnection syndromes of basal ganglia, thalamus, and cerebrocerebellar systems. Cortex; A Journal Devoted to the Study of the Nervous System and Behavior, 44(8): 1037-1066. DOI: 10.1016/j.cortex.2008.04.004.
Caruso, P., Moretti, R., & Manganotti, P. (2015). Speech disorder and behavioral involvement in a thalamic stroke: A case report. International Journal of Brain Disorders and Treatment, 1:007. https://clinmedjournals.org/articles/ijbdt/international-journal-of-brain-disorders-and-treatment-ij bdt-1-007.pdf
Kosif, R., & Izzet, A. (2016). The thalamus: A review of its functional anatomy. Medical Research Archives, 4(8). https://journals.ke-i.org/mra/article/view/740
Schmahmann, J. D. (2003) Vascular Syndromes of the Thalamus. American Heart Association Journals, 34(9): 2264–278. https://www.ahajournals.org/doi/full/10.1161/01.STR.0000087786.38997.9E
Brain Injury Explanation. (2015). Thalamus. https://www.braininjury-explanation.com/consequences/impact-by-brain-area/thalamus
Martini de Oliveira, A., Radanovic, M., Homem de Mello, P. C., Buchain, P. C., Vizzotto, A. D. B.,
Celestino, D. L., Stella, F., Piersol, C. V., & Forlenza, O. V., (2015) Nonpharmacological interventions to reduce behavioral and psychological symptoms of dementia: A systematic review”, BioMed Research International, vol. 2015, Article ID 218980, https://doi.org/10.1155/2015/218980
For more TBI Glossary Terms, click here.